Definition
Inflammation of the muscle attachments and interosseous membranes to the tibia (shin bone) on the inside of the front of the lower leg. Note: “shin splints” is a very widely used phrase and can refer to several lower leg injuries. The focus of this description is specifically on the inflammation described above.
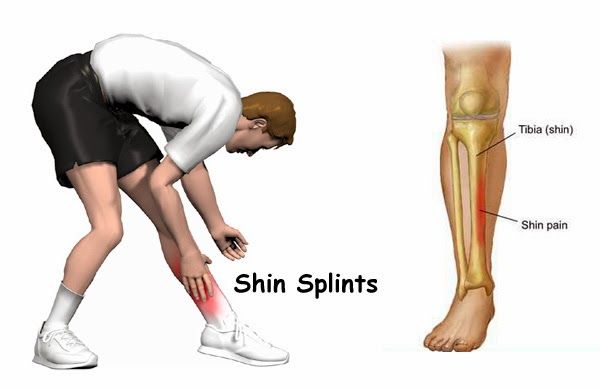
Symptoms
- Pain or tenderness along the inside of the shin, usually about halfway down the shin. Pain and tenderness may extend to the knee
- Pain on palpation of the shin
- Pain is most severe at the start of a run, but may disappear during a run, as the muscles loosen up. This is different to a stress fracture, where there is pain during weight bearing activities (walking, stair-climbing)
Causes
- Inflexible calf muscles and tight
- Achilles tendons – place more stress on to the muscle attachments
- Overpronation (feet rotate too far inward on impact) excessive running on hard surfaces, such as concrete pavements
- Incorrect or worn shoes
- Overtraining, or a rapid increase in training load or intensity
- Beginner runners are more susceptible to this problem for a variety of reasons, but most commonly due to the fact that the leg muscles have not been stressed in such a way before they started running.
Shin Splint – Treatment Methods
Self-treatment
- Stop running, especially in the case of severe pain, if pain is mild, then reduce training load and intensity, and avoid downhill running and running on cambered surfaces
- Take a course (5 – 7 days) of non-steroidal anti-inflammatory drugs(ibuprofen/voltaren/cataflam/mobic) available from your general practitioner or pharmacist
- Apply ice to the shin area – for 10 minutes every 2 hours, in order to reduce the inflammation
- Self-massage, using arnica oil or an anti-inflammatory gel, to the muscle only (along the inside of the shin).
- Stretching of the gastrocnemius and soleus muscles. Hold for 30 secs. Relax slowly. Repeat to opposite side. Repeat stretch 2 – 3 times per day.
- Remember to stretch well before running
- Return to running gradually
- Full recovery is usually between two to four weeks
Medical treatment
- Physiotherapy, if injury doesn’t respond to self-treatment in 2 to 3 weeks
- Orthotist or podiatrist for custom-made orthotics to control overpronation
- Orthopaedic surgeon – if injury does not respond to physiotherapy treatment, a bone scan, diagnostic ultrasound or X-ray may be necessary to check for a stress fracture.
Alternative exercises
- swimming, pool running, cycling (in low gear) “spinning”
- avoid any weight-bearing exercises
Preventative measures
- Stretching of the gastrocnemius and soleus muscles. Hold each stretch for 30 seconds, relax slowly.
- Repeat stretches 2 – 3 times per day. Remember to stretch well before running.
Strengthening of foot and calf muscles
- Place a weight around the foot, and move your foot up and down from the ankle, with no movement in the rest of the leg. Or use a partner to grasp the foot and provide manual resistance.
- Band exercises. Anchor one end of an exercise band (e.g; inner tubing of bicycle) to a heavy object, such as the leg of a couch. Loop the other end around the foot. Move the foot up, down, and from side to side against the band’s resistance to exercise different muscle groups.
- Correct shoes, specifically motion-control shoes and orthotics to correct overpronation
- Always apply ice after running
- Run on soft surfaces
- Avoid overstriding, which places more stress onto the shins
- Gradual progression of training programme
- Incorporate rest into training programme







